STROKE PREVENTION FOR AF
STROKE RISK FROM AF
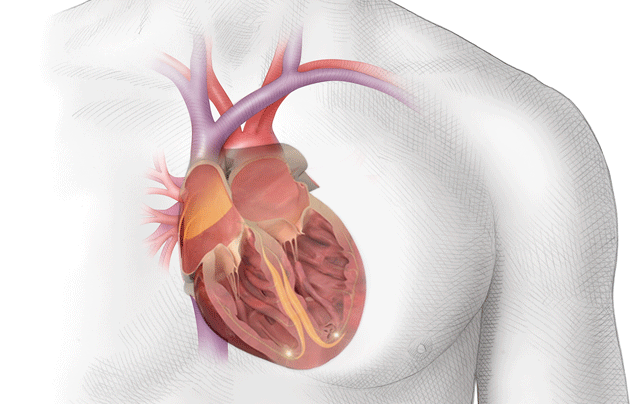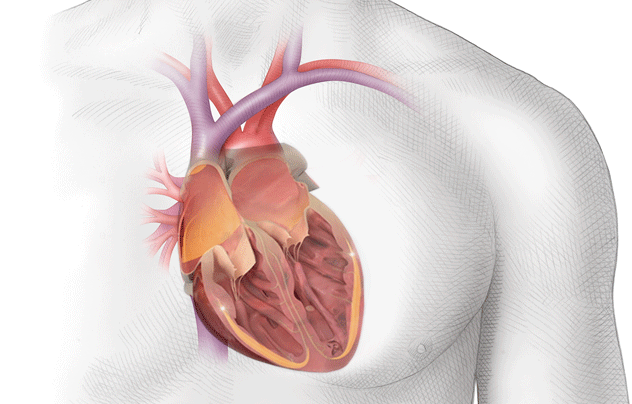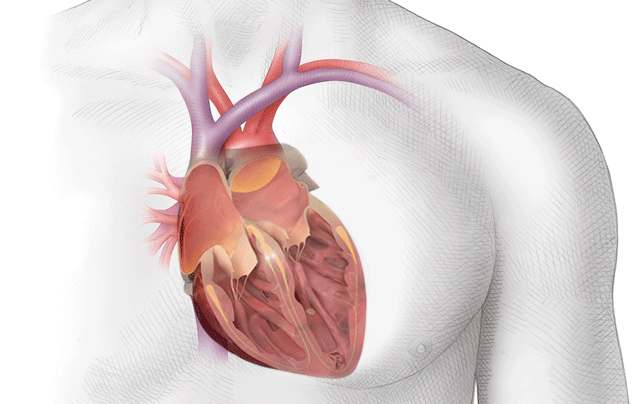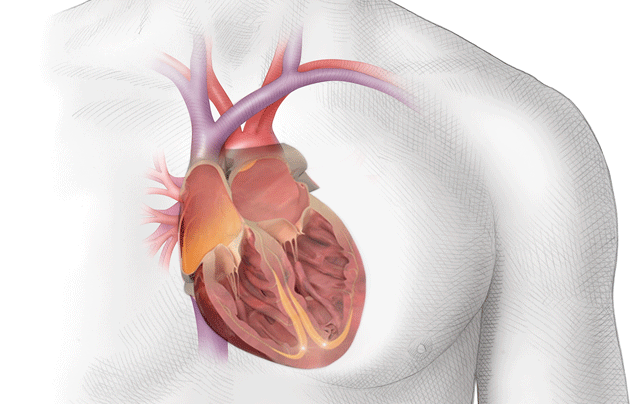
During atrial fibrillation the upper chambers of the heart quiver rapidly instead of their normal pumping action, which may allow blood to stagnate, and blood clots to form inside the heart.
The majority of blood clots form within a blind-ending pocket (called the left atrial appendage) attached to the left upper chamber. If a blood clot dislodges and travels to the brain a stroke may result.

WHO IS AT HIGHEST RISK?
Some people may go through their lives with AF and never have a stroke, but yet others will. Several characteristics increase a person’s risk of having a stroke – these include:
-
History of high blood pressure, even when treated
-
Diabetes,
-
Increasing age (in particular >65 years old),
-
Heart failure or weakened heart pump function,
-
History of a prior stroke or TIA (transient ischaemic attack),
-
Vascular disease of the arteries,
-
Female gender (age-related risk if >65 years).
These characteristics are termed risk factors and make up the CHA2DS2-VASc score (see below) that is used to guide treatment decisions for stroke prevention.
In general, the more risk factors the higher the risk of stroke. The risk of having a stroke each year varies from around 1% for people with no risk factors through to about 23% for a person with all of these characteristics.
CHA2DS2-VASc STROKE RISK SCORE
The CHA2DS2-VASc score is a stroke risk stratification tool in patients with atrial fibrillation (who do not have Rheumatic heart valve disease) and is used to determine the level of anticoagulation therapy required. The higher the score, the greater the risk of stroke.
The CHA2DS2-VASc scoring table is shown below. Adding together the points that correspond to the patient’s conditions will result in a score that is used to estimate stroke risk:
A CHA2DS2-VASc score of 2 corresponds to an annualised stroke risk of >2%. A score of 2 or greater is considered to be a 'high' long term risk of stroke.

STROKE PREVENTION TREATMENTS
There are currently 2 options to prevent stroke for people with AF – “blood thinner” medications or a procedure to seal off the left atrial appendage (left atrial appendage occlusion). Recommended treatments vary according to a person’s risk of stroke and bleeding.
'Blood thinner medications (also called Oral Anticoagulation) are the mainstay of therapy to reduce the risk of stroke from AF. Oral Anticoagulation options include newer medications (sometimes termed NOAC or DOAC) such as Dabigatran (Pradaxa), Rivaroxaban (Xarelto), Apixaban (Eliquis) and also an older medication warfarin (also called VKA or brand names Marevan or Coumadin). Warfarin (VKA) is the recommended treatment for patients with 'Valvular AF' which refers to rheumatic mitral valve disease or mechanical heart valve replacement. The following are International Guidelines with recommended stroke prevention for patients with AF according to their risk score:

MYTH
It is not necessarily true that the more AF you have then the higher the risk of stroke. A person who has only a few episodes per year can still have a stroke, whereas another person in “full-time” AF may not. Being in normal rhythm rather than AF does not necessarily reduce the risk of blood clots and stroke. Stroke risk is best estimated by the CHADS2-VASc score.
HOW EFFECTIVE ARE THE TREATMENTS?
Less than one quarter of all strokes are caused by AF. In fact, the majority of strokes result from hardening of the arteries (atherosclerosis) leading to the brain and the effects of high blood pressure.
Different treatments are often required to lower the risk of stroke from these conditions. Although no treatment is 100% effective, patients with AF can significantly reduce their chances of having a stroke with appropriate therapy.